Telehealth is often associated with remote video consultation applications in which doctors and patients meet over videoconference. In reality, however, the telehealth — also known as telemedicine — ecosystem encompasses the delivery of health-related services through technology, which can include medical care, health education, and healthcare information services. Some examples of Telehealth platforms are: mobile health apps, personal monitoring devices, video conferencing apps, digital patient portals, and healthcare educational sites.
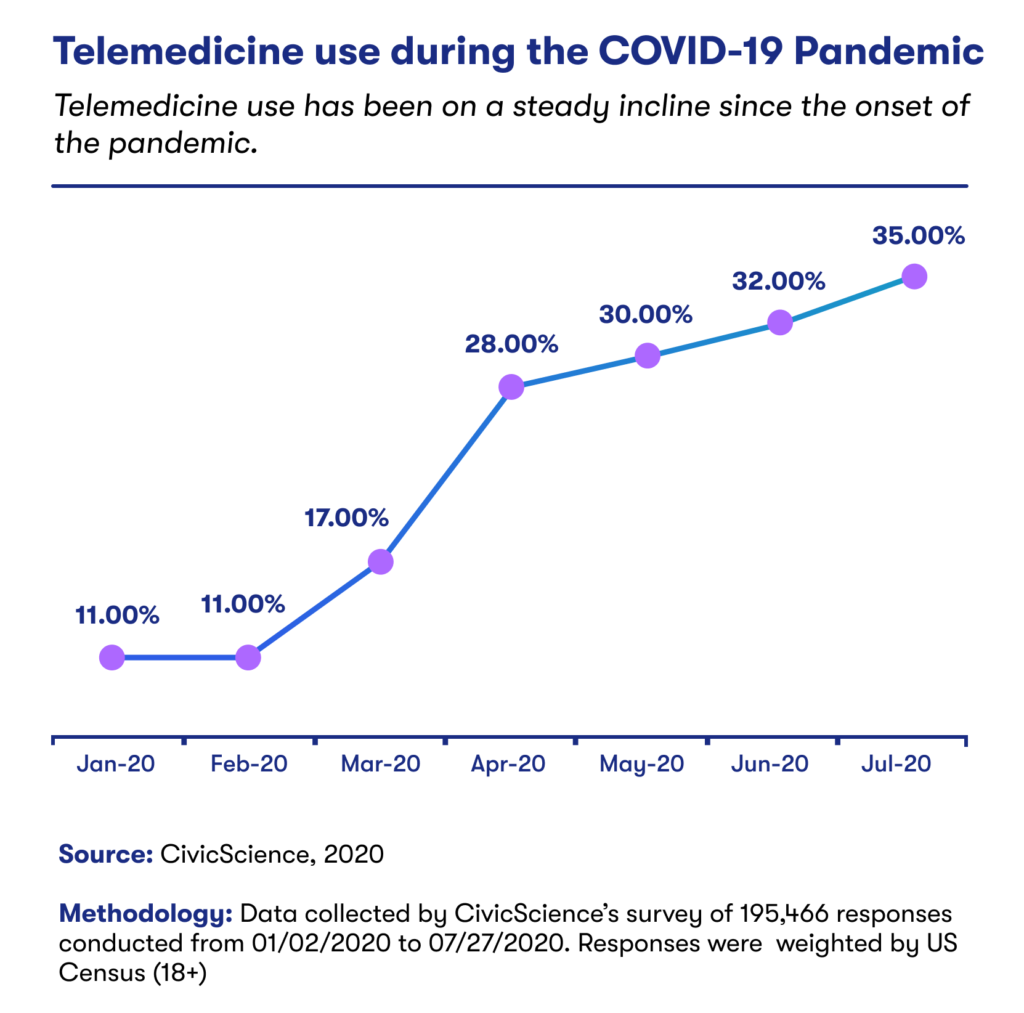
The COVID-19 pandemic rapidly accelerated the digital transformation of the U.S. healthcare system through 2020, and as such telehealth is expected to be a key area of disruption in the next decade.

Main components of a telehealth application

1- The Frontend, ie mHealth applications
The frontend, which normally refers to mHealth or Mobile Health solutions. These applications can be accessed from mobile devices or a computer connected to the internet. This is the visual part of the platform in which the patient can schedule consultations, access real-time health data or PHI (protected health information), run videoconferences, see reports and analytics, get health tips and recommendations, or set medication reminders.
Key: the importance of UX/UI Design
The interaction and interface design of these applications is crucial for the overall success of the entire experience. The wide range of requirements that a diverse audience brings, the importance of showing precise health analytics, and the need for secure and fast interactions amount to a significant challenge for both the software development and design teams who build these products.
Frontends for Doctors, MP, and general medical staff
The frontends for this audience are much more focused on information access, data analytics, and organizational administration. When transitioning from legacy software platforms, note that it is much easier to implement desktop web applications than mobile native applications given that doctors and medical staff are often located inside a healthcare organization with a wide range of security protocols.
2- The Backend, ie Store-and-Forward technologies
The backend component of the platform, which runs on secure servers and is responsible for the storage and transmission of PHI.
Key: Security and data management
The security and reliability of these platforms are of central importance. The software must be architected such that the system can guarantee that patient data will be available 24/7 without the risk of being compromised.
There are standards and certifications like HIPAA or HITRUST that guide healthcare software development teams on how to develop and maintain software platforms that manage sensitive patient information. These standards usually refer to a set of conditions that have to be met by software platforms, business operations, and physical infrastructure.
Historically health organizations managed their physical servers, placing them in private, secure locations. More recently, the proliferation of cloud-based hosting has meant that organizations’ infrastructure can now run securely within vendors like AWS or Azure. As is the case across most other industries, the cloud will likely become the de facto solution for telehealth as well.
3- Remote patient monitoring (RPM) devices
Smart remote health monitoring devices are becoming increasingly common. They grant their users real-time access to a wide variety of health stats such as oxygen levels, blood pressure, respiration rate, heart rate, stress levels, sleep patterns, and more.

The early detection of concerning indicators such as an irregular heartbeat can prevent serious problems before they happen.
RPMs are responsible for data collection, transmission, and evaluation, and in some cases will send notifications to patients and health providers.
The ever-widening user base for these devices represents exciting opportunities for population-wide evaluations of ailments and health outcomes. However, data privacy and security must be baked into any of these efforts at a fundamental level.
Employers and RPM devices
Around 11% of employers added wearables to their wellness plans with the goal of incentivizing healthier behavior among employees in order to reduce medical costs and improve employee health.
Medical evaluation kits
Telehealth technologies have also enabled patients to gather samples, such as a drop of blood, at home, ship that sample to a lab, and then review the lab results with a qualified professional, all without ever having to leave the house. The COVID-19 pandemic has highlighted the importance of this model.
Catapult Health, a leading preventive care company and one of our healthcare clients, gives employers an easy way to take care of their employees by delivering health evaluation kits directly to each employee’s home, followed by a video conference with a Nurse Practitioner who reviews the lab results and provides a plan to address any issues. This was essential to Catapult’s business during the past year.
The challenges ahead
The main challenges for software companies building the next generation of telehealth apps are related to platform interoperability, data security, and customer privacy.
The most challenging of these from a technical perspective may very well be interoperability. As more players enter this space, disparities in both the types of data tracked and the concepts underpinning the systems will continue to grow. Both of these forms of fragmentation equate to more complexity when trying to share information, and there is little incentive for companies to address the issue.
In the following article, we will touch on the different protocols and standards that aim to improve the interoperability between platforms.
About us
Qubika is a software development company that is currently working on the next healthcare platforms for organizations that are paving the way in the industry. To learn more about our services visit: qubika.com


























